Monday, February 28, 2011
Hope
Thursday, February 24, 2011
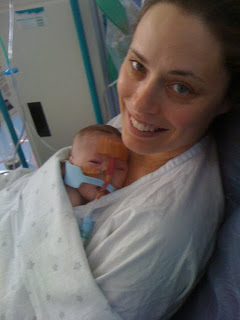
Our first cuddle
Wednesday, February 23, 2011
Thursday, February 17, 2011
Wednesday, February 16, 2011
hanging in
Tuesday, February 15, 2011
Monday, February 14, 2011
Baby-ish
Thursday, February 10, 2011
Sullivan Slideshow
 These photos were taken by Helen Roberts when Sully was 4 days old. We thought we were going to lose him that day...the hospital provides a photographer free of charge for families of critically ill babies. Click on the photo to view a flicker slideshow of a few more of these beautiful pics.
These photos were taken by Helen Roberts when Sully was 4 days old. We thought we were going to lose him that day...the hospital provides a photographer free of charge for families of critically ill babies. Click on the photo to view a flicker slideshow of a few more of these beautiful pics.
Visit from Captain(s) Starlight
Wednesday, February 9, 2011
EBM
Expressing is weird, especially at first, the midwives helped me "hand express" first to bring the milk in (literally, I was so tried I let them touch my boobs). They used a syringe to catch the first bit and eventually I was ready for the pump. I was really worried about whether I would be able to produce milk with all the stress, but it is going well so far. I think the most important thing I have done is stick with it, I almost gave up one day because Sully was having such a hard time. I was exhausted, stressed, and missed a whole day just because everything was so full on. It was Neil who really encouraged me and also one of the midwives on the ward. She simply said, you don't have to do it--it is something you should do only if you want to.
Keep fighting Sully!
Most adults wouldn't survive what Sul is going through right now. Our surgeon says that babies are more resilient than adults. Sully has a tube down one nostril going to his stomach, the ventilator down the other nostril, an IV in one hand, one foot and in both inner thighs...he has just a bit of lung but still tries to breath over the ventilator when he can and has had major surgery to rearrange his guts...now he is fighting a blood infection and pneumonia. I can feel how strong he is when I sit beside him and hold his hand.
Dig deep little one...
Monday, February 7, 2011
step forward step back
Sent from my iPhone
Sunday, February 6, 2011
Look Mom no nitric oxide
Friday, February 4, 2011
Wretching
Thursday, February 3, 2011
Rocky days ahead
Wednesday, February 2, 2011
transition from sprint to marathon

 The past couple of days have been rough for me and Sully. He has had some difficulties with the ventilator - bit complicated for me to try and explain but one issue was he was trying to breathe on his own and got upset and hyperventilated which caused a bunch of problems. At the same time, the ventilator was not calibrating properly and well, it was just a couple of days of up and downs. When Sullivan gets stressed his pulmonary hypertension (too much pressure in his lungs) gets worse and his blood desaturates (gets less oxygen) which is bad. And when Sully's is stressed, I am stressed. Today has been a much better day so far, he tolerated getting turned on his belly and the doctors are weaning him off some drugs including sedation so he will wake up a bit more. He needs to be more awake to cough, cry (without sound because of ventilator), and wiggle to move fluid out of his lungs (amongst other benefits). It is hard for me to see him cry and not be able cuddle him. During the last two days I have started to come to terms with what it really means to have a really sick bub and that as a parent there is not way ever of taking away a child's pain...no magic wands! Anyway, Sully's is a little soldier that's for sure. I bought him some new hats and decorated his room to lift my spirits.
The past couple of days have been rough for me and Sully. He has had some difficulties with the ventilator - bit complicated for me to try and explain but one issue was he was trying to breathe on his own and got upset and hyperventilated which caused a bunch of problems. At the same time, the ventilator was not calibrating properly and well, it was just a couple of days of up and downs. When Sullivan gets stressed his pulmonary hypertension (too much pressure in his lungs) gets worse and his blood desaturates (gets less oxygen) which is bad. And when Sully's is stressed, I am stressed. Today has been a much better day so far, he tolerated getting turned on his belly and the doctors are weaning him off some drugs including sedation so he will wake up a bit more. He needs to be more awake to cough, cry (without sound because of ventilator), and wiggle to move fluid out of his lungs (amongst other benefits). It is hard for me to see him cry and not be able cuddle him. During the last two days I have started to come to terms with what it really means to have a really sick bub and that as a parent there is not way ever of taking away a child's pain...no magic wands! Anyway, Sully's is a little soldier that's for sure. I bought him some new hats and decorated his room to lift my spirits.
Me
 I finally had the courage to leave the hospital grounds Sunday morning. Neil and I had a chat with one of Sullivan's doctors, and to be perfectly honest I needed to ask if we had minutes, hours, days to get to the hospital if Sul's condition started to deteriorate. The doctor said days, and that everyone, including us, would be able to see what was happening. He was very kindly and told me I looked exhausted and needed to go home to rest. I was a bit teary when Neil took this pic but we had a plan to go back for an evening visit. I am feeling a better having slept in my own bed, and have had a couple of naps. We call the ICU nurse whenever we feel like it to get an update on how is is going so we call every few hours including in the middle of the night, so we sleep a bit easier.
I finally had the courage to leave the hospital grounds Sunday morning. Neil and I had a chat with one of Sullivan's doctors, and to be perfectly honest I needed to ask if we had minutes, hours, days to get to the hospital if Sul's condition started to deteriorate. The doctor said days, and that everyone, including us, would be able to see what was happening. He was very kindly and told me I looked exhausted and needed to go home to rest. I was a bit teary when Neil took this pic but we had a plan to go back for an evening visit. I am feeling a better having slept in my own bed, and have had a couple of naps. We call the ICU nurse whenever we feel like it to get an update on how is is going so we call every few hours including in the middle of the night, so we sleep a bit easier.
First Feed


Sully had his first poop 3 days after surgery (Monday) so we had the green light to go ahead and try a feed - 2 mls of breastmilk every 4hrs. Sully tolerated this very well we are very excited that his guts are working in their new position! I have been expressing milk every 3hrs during the day and 4 hourly in the night. I owe a entire post to expressing milk so I will leave the details for now. If we are at the hospital for the feeds, Neil and I are given the task of pushing the syringe of liquid gold through Sully's feeding tube, which goes through his nose into his stomach. The nurse checked that it was absorbed by putting a syring back on the tube 2hrs after the feed and pulling up to see if any was left in his belly. Sounds gross but thought someone out there may be wondering.